Multidisciplinary Team Cluster development
294 people supported through a multidisciplinary approach
The transformational work around the Cardiff Southwest Cluster has seen significant improvements in patient care with fewer unplanned hospital attendances clearly demonstrated in comparison to other clusters.

Find out more about the work of the South West Cluster
Feedback about the service:
From people using the service
“It has helped me so much and I now feel I’m getting somewhere. I am now in touch with the people who can help me recover. Thank you.”
“I have met many people and attended groups at the dusty forge, everyone has been very supportive.”
“Amazing service, I felt a lift when a message was left … I feel so assured there’s someone out there for me.”
From staff:
“The ability to refer to the wellbeing team have been transformational, it has allowed us to de-medicalise problems that are social or due to wellbeing.”
“Using the elemental system for referral has been very positive and helped increase referrals as it is much easier to refer to one central place rather than trying to remember which form to use.”
“The work reconciling medications and contacting patients on discharge has been very welcomed, patients really appreciate having a telephone from the Hub on discharge and it often is timely to pick up issues they may be having once discharged”
Integrated Discharge Service
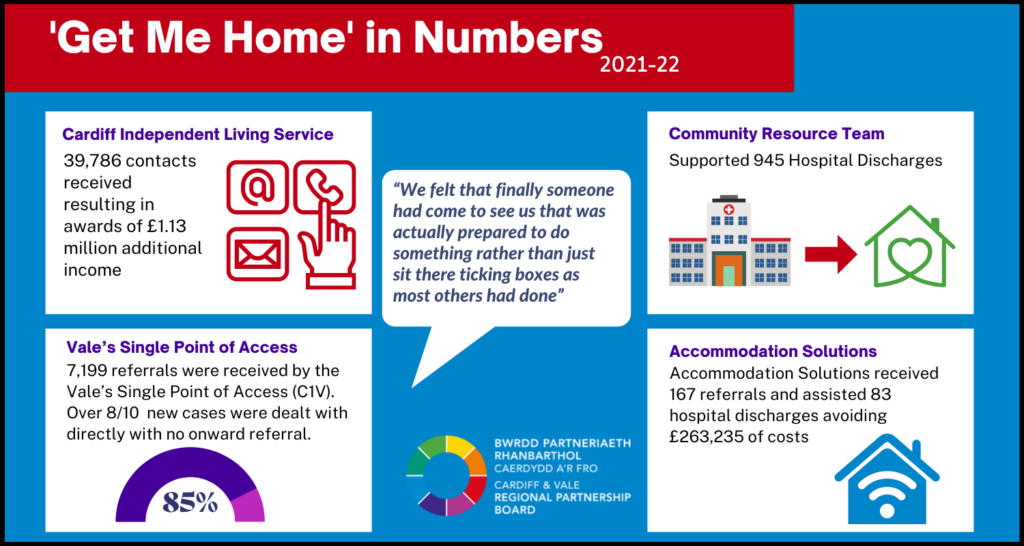
Supported 945 people with discharge through our community resource and extended ‘bridging’ teams
Over the past year, our hospitals have seen significant pressures due to the ongoing pandemic. This was particularly highlighted over the winter period, when both increased presentations in hospital along with reduced access to care and support in the community, meant that coordinating discharge became a priority in order to keep people safe.
The RPB ICF Integrated discharge service worked alongside the Transformation Fund Get Me Home project to assist in coordinating discharges as soon as possible by having teams in the hospital coordinated with community resource, social services, third sector and other community support services to ensure people had the support in place to return home safely.
Feedback from ward staff:
“They are a hard-working caring group of professionals and are a big help in promoting wider patient flow…particularly in the context of wider constraints aggravated by Covid.” (Consultant Geriatrician)
“There is improved communication on the ward between health staff and social services in regards to waiting on information around package of care and communication to social workers.” (Occupational Therapist)
“Having support is leading to efficient, safe discharges and reducing the amount of time patients are in hospital. As a new ward manager I have learnt and been guided by the FPOC team.” (Ward Manager)
Feedback from staff involved with service:
“It’s great being able to genuinely make a small difference to peoples’ experiences in hospital and reassuring them that they are not alone… We make sure they stay connected with their community and with the things that are important to them.”
“I work with a wonderful team of like-minded people across UHW, who come together to help patients to achieve what matters to them most.”
“I enjoy the board rounds working in a cross-cutting team, problem solving with our health colleagues and sharing knowledge of the community to get the best solutions for a patient and optimal discharge.”
Improving Access to Services
129,451 calls across our access services in Cardiff and Vale of Glamorgan, who dealt with most enquiries at first contact so issues were quickly resolved.
A key focus for our @Home programme, as well as for the Integrated Care Fund (ICF), was to make access to services simpler, with fewer referrals and a multi-disciplinary team approach. This has been successful with our ICF projects and is one of the foundations for our new programme of work.
Find out more about how services work together to wrap care around the person.
Find out more about Ageing Well
Our Priorities

DECHRAU’N DDA
STARTING WELL
We want every child in Cardiff and Vale to have the opportunity to thrive. Our work focuses on children in vulnerable situations and the services that support them.

HENEIDDIO’N DDA
AGEING WELL
We know how hard it can be to find help when people need it the most. We want to make sure there is community support to help people stay as healthy as possible so they can carry on doing the things that matter most to them.

BYW’N DDA
LIVING WELL
As a Partnership we have worked together with people with a learning disability, their families, carers and the third and independent sector to produce a clear direction for the planning and delivery of adult learning disability services across the region over the next five years.
